The Artificial Urinary Sphincter is the gold standard NICE approved treatment for Stress Male Urinary Incontinence. This device has been in clinical practice for over 40 years and has excellent long term results. The Artificial Urinary Sphincter consists of 3 separate pieces that are interconnected and are placed in the perineum (area between the testicles and anus), the scrotum and abdomen. This either cures or significantly improves stress urinary incontinence in over 90% of patients. One of the Manchester Urology surgeons is part of the North West Reconstruction and Implant Centre and regularly places the Artificial Urinary Sphincter. He is also a member of the British Association of Genito-Urinary Reconstructive Surgeons and involved in National Research into the management of Male Stress Incontinence.
With a thorough history, examination and investigations the severity of stress incontinence is diagnosed. It is often graded as mild, moderate or severe. The Artificial urinary Sphincter is the only recommended treatment for moderate to severe stress incontinence, although there is a National Randomised Controlled Trial looking at alternatives in the mild to moderate group of patients with male stress incontinence. Our Manchester Urology Consultant is a Principle Investigator in this trial.
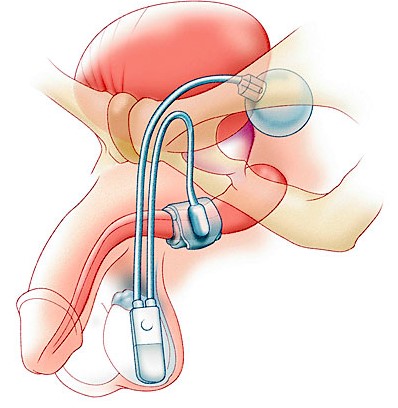
The Artificial Urinary Sphincter consists of 3 components See Figure 1.
1) The main part is a cuff that surrounds the urethra (water pipe). When activated this compresses the urethra to prevent urine leakage.
2) The cuff is connected to a pump in the scrotum. This is the part of the device that the patient uses to cycle (use) the device and the specialist can use to deactivate and deactivate the device.
3) A fluid filled reservoir (balloon) is placed in the abdomen and tubing connects all 3 pieces of the device together.
When placing the device it is important that the cuff size is chosen very carefully as if it is placed too tight it could cause erosion but conversely if placed to loosely then it may not work as effectively.
Figure 1. Diagram of Artificial Urinary Sphincter
Patient information: what to expect
One week before the operation you will be asked to provide your GP with a urine sample to ensure there is no infection. If there is infection the procedure would need to be deferred as one of the most significant risks is infection of the device. You will also require a preoperative assessment. If you are on any anticoagulant medication (blood thinning medication) you will be advised at the preoperative assessment about when you should stop these.
You will be admitted on the day of surgery where your surgeon and the anaesthatist will see you. You will often have completed the consent form before the day of surgery but your surgeon will go through this again to ensure you understand the risks of surgery (please see Patient Information Sheet for more information on specific risks).
You will be given intravenous antibiotics during and after the procedure and then sent home on oral antibiotics.
The procedure is often carried out under general anesthetic but sometimes a spinal anaesthetic is used. There will be a small incision in the perineum (area between the scrotum and the anus) to allow the placement of the cuff around your urethra. A separate incision is made in the groin to position the pump, and the balloon reservoir is inserted behind the abdominal wall through the same groin incision.
When you wake up you will have a catheter in (plastic tube in your penis) and this is removed the following day. The average length of stay is 48 hours. When the catheter is removed you will still be incontinent as the device has been deactivated. This is to allow recovery from the operation before use. It is important to try and keep the incisions as clean and dry as possible.
At about 6 weeks you will be seen back in clinic for the device to be activated and for you to be shown how to use the device.
The following videos show firstly an animation on how to cycle the device and secondly what the cuff looks like from the inside of the urethra while being cycled.
Video 1: Animation of Artificial Urinary Sphincter being cycled.
Video 2: View of the cuff around the urethra being cycled.
For more information please see the Artificial Urinary Sphincter Patient Information Sheet. If you would like to see a Manchester Urology Surgeon to discuss the Artificial Urinary Sphincter in more detail then please call 01614957796.
Information leaflets
http://www.baus.org.uk/_userfiles/pages/files/Patients/Leaflets/AUS14.pdf
Links
http://www.baus.org.uk/_userfiles/pages/files/Patients/Leaflets/AUS14.pdf